It is insufficiently known that when asked, patients are very willing to share their medical information with researchers but much less so with public health authorities or third party companies. It is therefore ironic, that whereas the latter two groups do not require institutional review, researchers do. Moreover, if a study pertains to a set of patients seen at different institutions, the researcher will first have to obtain review from the institutional review boards (IRBs) of each one of the institutions. For a variety of reasons there is significant inertia working against getting one IRB to cede review of the study to another IRB. For this reason, this draft policy from the NIH is a welcome potential accelerant of biomedical research. If it is ratified, this policy will ensure that a single IRB for these multi-institutional studies becomes the rule and not the exception. A seemingly fine point to those who have never had to organize a multi-institional research study, but it might do more to advance medicine than hundreds of millions of dollars in additional research funding.
Harvard Medical School's Countway Library of Medicine and the new frontiers in biomedical computing
2014-12-04
2014-09-23
Worrisome Trends in Ebola
My colleague John Brownstein just shared these worrying projections for Ebola epidemiology.
2014-08-06
Near real-time tracking of Ebola
If you want to see just how Ebola is spreading (and soon regressing?) , this article provides the view and insight of how it’s done. Ten years ago, these data would percolate slowly, compiled by public health authorities and eventually appear in an academic or lay publication Now through the foundations of computational epidemiology established by Dr. Brownstein, we are able to directly monitor this in-progress disaster. Now that we have a good afferent circuit, let’s see hope the efferent circuit is even more robust.
2014-03-27
Classification system worthy of legislative intervention?
The ICD-10 diagnostic classification system is due to be adopted by US healthcare systems this year. However, new legislation would defer that change by at least a year. Who would have thought that a group of statisticians working on a list of the causes of death in 1891 would cause billions of dollars to be spent and thousands of hours invested in debating what that list should look like?
This fine system of classification that would have made Linnaeus’ head spin includes classic diagnoses such as:
V91.07xD (burn due to water-skis on fire, subsequent encounter)
W56.22xA, (struck by orca, initial encounter.)
W56.12XA (getting struck by a sea lion)
V97.33XD (Sucked into jet engine, subsequent encounter)
The orcas may have to wait another year before getting their medical recognition.
2014-03-25
Achieving clarity in cancer genomics
Approximately 3 years ago, we held a clinical bioinformatics summit to discuss with international leaders in genomics, genetic testing and clinical laboratory procedures what it would take achieve clinical grade whole genome sequencing (WGS). That is to make WGS a safe and useful component of routine diagnostic assessments in the clinic. Among the mechanisms we chose to accelerate the advent of clinical grade WGS was a competition where 3 families contributed their genomic sequence and clinical histories. Then multiple teams assembled and competed to produce the most accurate, most clinically useful diagnostic report. The competition resulted in a lot of learning and multidisciplinary team formation but also, even though we had not dared count on it, several breakthrough diagnoses. A good lay summary can be found here from Bio-IT World and an in-depth scientific summary here. Also, the cake presented by one of the mother’s to her child, who had gone for years without a diagnosis until the leading teams converged on the same mutations in the same gene, is shown below. With generous funding from Rob and Karen Hale, we kicked off the next round of the CLARITY competition as described below.
In addition to rare undiagnosed diseases, perhaps the most clinically impactful area of genomics, in the near term, is that of precision diagnostics for cancer. However, the analytic challenge is far deeper as it requires analyzing tumors that are often heterogeneous (i.e. different clones), comparing it to germ line sequence (i.e. non-tumor DNA). Then, how are we to determine which of the mutations found are relevant to the diagnosis or therapy selection? Integrating information from RNA sequence and epigenetic modifications (e.g. DNA methylation) may help and there are several good ideas being proffered by several researchers. Yet, how do we begin to bring all the data together systematically and meaningfully for patients with a malignancy? Given how early we are in this new realm of medicine, we decided to first hold a workshop where several national leaders in cancer genomics gave thoughtful assessments of the best way forward. After we we synthesize the learning from this meeting, we will announce a new CLARITY challenge for patients with recurrent cancers. Shown below are some of the speakers at the meeting which included Gad Getz, Rick Wilson, Peter Park, David Sweetser, David Margulies, Isaac Kohane, Judy Garber, Sharon Plon, Steve Chanock, Marian Harris, Heidi Rehm, Levy Garraway, and Katie Janeway. Another small but important step forward in the development of a data-driven, computationally-enabled medicine.
2014-03-03
Scholar Medical Publication DIY by Harvard Medical Students
If, as F. Scott Fitzgerald is reported to have said, action is character, then the current crop of Harvard medical students are impressive characters. Amid all the din about who controls publication, open access and shortening the loop between academia and public dissemination, a small group of determined individuals have just come out with their premiere issue of Harvard Medical Student Review. Considerable forethought, extensive deliberations with HMS leadership and creative talent have produced what is likely to become an authoritative voice for medical students and those interested in medical education and science. In the words of the student publishers themselves:
Today we are introducing the Harvard Medical Student Review, an online journal that will serve as a forum for students to participate in the conversations on healthcare and medicine. Our classmates here and around the world come from innumerable backgrounds, rich in thought-provoking experiences; we have much to share. Topics may range from research to reflections on training and experiences with patients. We hope that through writing and reflection, we can spark productive debate, generate innovation, and learn from one another at the beginning of our professional education and careers.As members of the medical community, we have a duty to review the facts and communicate the truth with clarity, precision, and humanity. In his address at the 2012 Harvard Medical School commencement ceremony, Dr. Don Berwick called upon new physicians to wield their voices proudly in carrying out this duty, as each voice “can be loud, and forceful, and confident, and will be trusted.” [2] The Harvard Medical Student Review is a space for students, trainees, and professionals to answer that call.We hope you will join us.
2014-01-24
Battle of the beauty contests
So how best to have a public debate about how we allocate the public monies for biomedical research?
.
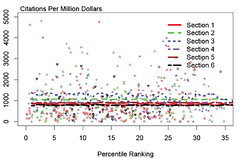
Hat tip: David Osterbur.
2014-01-23
Welcome news from the Wellcome Collection
Many of us have had the following experience. We find an interesting illustration and use it for a scholarly presentation or for a class. Then a well meaning compliance officer will notify us that if we are going to put the presentation on the web, we will have to secure the rights to the illustration for that purpose. Often the expedient response is to delete the illustration or withdraw the entire presentation from the public domain.
In this context this British invasion is a hopeful glimpse of the future. One hundred thousand pictures were just made freely available (so long as you correctly attribute their provenance). So, if you want to illustrate Harvey’s anatomical exercises of the heart and circulation, or contrast modern medical advertising to that of a well regarded phrenologist, the materials are there for you (see below), for free and without any administrative overhead. The other flank of the British open access image invasion is led by the British Library from which the charming picture below of the anatomy of the leech was taken.











